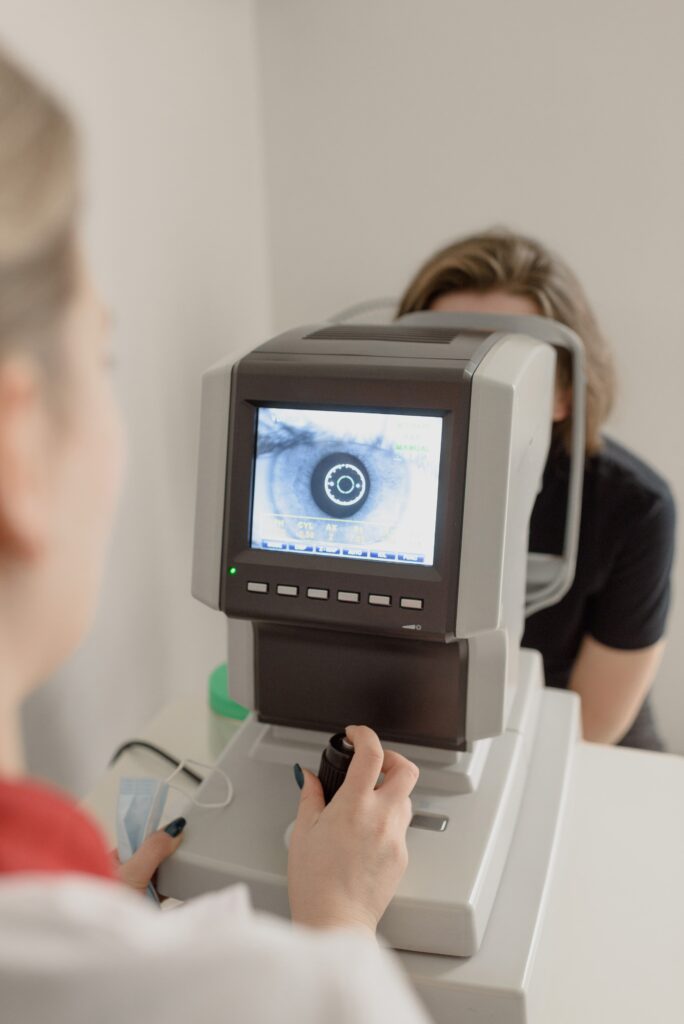
Glaucoma: The Subtle Threat to Eyesight
Glaucoma is not just an eye disease; it is a group of eye disorders that damage the optic nerve.
The optic nerve serves as the data cable of the eye to the brain. Inevitably, when the line is damaged, it cannot provide the brain with the entire picture, leading to vision loss.
Glaucoma often occurs from the build-up of normal fluid (aqueous humor) being over-produced or improperly drained from the eye.
Typically, the fluid drains into the trabecular meshwork and absorbs into the bloodstream. However, too much aqueous humor or a failure in the drain system increases pressure in the eye, which damages the optic nerve.
There are several forms of glaucoma, but the two primary types are open-angle and narrow-angle.
Primary open-angle glaucoma (POAG) is the most common form diagnosed. The second most common type of glaucoma is Narrow-angle glaucoma (NAG).
Narrow-angle glaucoma occurs when the angle of the eye (found where the iris and cornea meet) becomes constricted; this can happen because the crystalline lens grows and expands throughout life, and eventually, it pushes the iris toward the cornea. People over the age of 40, women, hyperopic (near-sighted) patients, and those of African, East Asian, and Inuit descent carry an increased risk of this variant.

Angle-closure can occur from the constriction of the pupil during dilation, which is why eye doctors check eye pressure, screen the openness of the angle, and check for other signs of glaucoma before a dilated eye exam. However, angle-closure can also occur from the natural dilation of the eye, so it’s imperative to be aware of its symptoms and immediately contact an ophthalmologist or emergency room if you experience them. The symptoms of angle-closure are severe headache, eye redness, nausea or vomiting, extreme light sensitivity, and blurred vision.
Another somewhat less common type of glaucoma is normal-tension glaucoma. Normal-tension or low-tension glaucoma acts very similarly to primary open-angle glaucoma, but it does not elevate the pressure within the eye. Researchers are still unsure how this variant damages the optic nerve, but they believe it is from poor blood flow to the optic nerve.
What are the symptoms?
Glaucoma harms the eye silently and is only detectable through an eye exam. Apart from drastic vision loss, the damage is only recognizable through inspecting the optic nerve and gauging eye pressure. If anything abnormal stands out during the exam, your eye doctor will schedule more in-depth tests to determine if glaucoma is present.
Due to its subtle nature, yearly eye exams are crucial, especially for those sixty and older: since glaucoma damage is irreversible, early detection is vital.
What are the contributing risk factors of glaucoma?
Family history:
Nearly half of all glaucoma cases are familial, most connected to siblings. Notably, individuals who have a sibling diagnosed with glaucoma are about 10 times more likely to develop the disease themselves. So if glaucoma runs in your family, be sure to tell your eye care provider during your next eye exam. Likewise, if you are diagnosed with glaucoma, encourage your family members to see their eye care provider(s) as well.
Age:
The risk for glaucoma increases with age, so those over 60 should have yearly eye exams. However, if you have a family history of glaucoma, consider having annual eye exams starting at age 40 as a preventative measure.
Ethnicity:
People of African or Hispanic descent are at an increased risk for developing open-angle glaucoma. New research is underway to understand why this occurs. Current understanding has linked genetic traits such as thin corneas, larger optic nerves, high blood pressure, and poor blood flow to the optic nerve as potential causes.
As mentioned earlier, those of Asian heritage are at a higher risk of developing narrow-angle glaucoma, with nearly 90% of cases of glaucoma-related blindness in China linked to narrow-angle glaucoma.
Medical conditions:
High blood pressure, heart disease, sickle cell anemia, and diabetes elevate the risk of developing glaucoma, so be sure to notify your eye care provider if you have a history of these conditions.
A few other risk factors:
Those with high amounts of myopia (near-sightedness) or hyperopia (far-sightedness), those who have a history of long-term use of certain medications, particularly corticosteroids, eye injuries, or even some eye surgeries, can also add the risk of glaucoma.
What can you do to prevent glaucoma?
There is not much you can do to prevent glaucoma. However, you can stay ahead of it and limit certain risks of developing it!
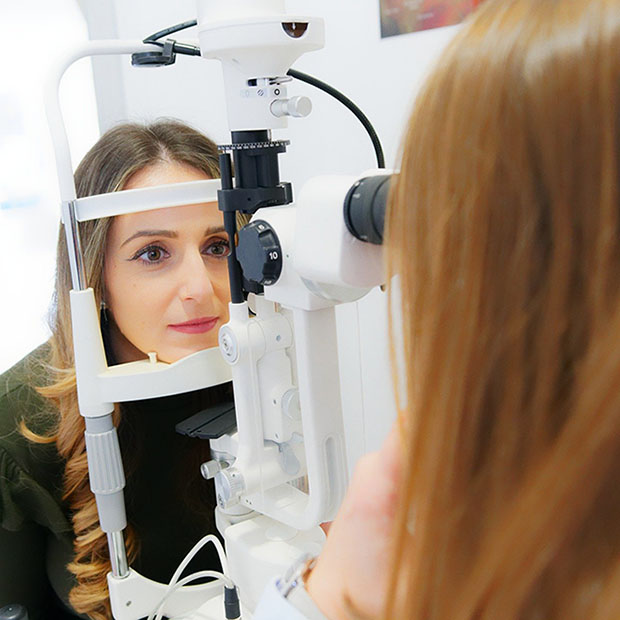
Schedule routine eye exams:
Routine eye exams are the most significant way to protect your eyes from glaucoma-related vision loss. Specifically, ask your optometrist for an iWellness scan – this test is simple and takes mere minutes to perform along with your routine eye exam. While insurance does not cover the cost of the scan, its benefits include the ability to detect forming eye diseases at least 5 years before they are detectable through a dilated eye exam. Preventative measures like the iWellness can give you a headstart in thwarting damage from glaucoma and macular degeneration.
Maintain a healthy diet:
A healthy diet can help prevent certain health disorders such as high blood pressure and diabetes, which increase the risk of developing glaucoma. While there is no strong connection yet, research is underway to determine the link between diet and glaucoma development. One study recently found that those consuming 3 servings of fruit and vegetables a week had a decreased risk of developing glaucoma.
Regular exercise:
Exercise is another means of preventing diabetes and heart disease, making it an eye-health benefit. Yet, glaucoma or elevated intraocular pressure (IOP) can limit certain routines; exercises like weight lifting or those that include inversions (downward dog in yoga) can raise eye pressure. Those diagnosed with glaucoma or elevated IOP should always speak to their eye care provider before diving into a new workout regimen.
Undetected glaucoma can cause irreversible vision loss, so early detection is the key to preserving eyesight.
To best guard against this silent vision threat, maintain a healthy lifestyle with a good diet and glaucoma-safe exercises. Also, be sure to discuss any pre-existing risk factors with your eye care provider and follow their recommendations for preventative care, including an iWellness scan. Schedule an eye exam at least every two years until the age of 40, and then modify your eye care schedule based on the recommendation of your eye doctor.